I estimate that one in every 10 people who come to me are suffering from panic attacks. They think they are going mad and berate themselves for feeling out of control. Yet panic attacks are not what you think. They are a stimulus-response circuit that your body has learnt. I have suffered from them myself. It limits lives, even ruins lives if left to run without help for long enough, becoming a panic disorder.
The symptoms include: feeling of faintness (or actually fainting), lightheadedness, chest pains, rapid breathing, rapid heartbeat, numbness, sweating, tingling feeling on the fingers, nausea, hot flashes, trembling or shaking, abdominal pains. A feeling that you are about to have a heart attack or die. People can feel like they are about to vomit, or have diarrhoea. Symptoms vary from person to person, but they are very frightening.
Who gets panic attacks?
Panic attacks can happen to anyone. Many of us may have had one or two in our lives, and overcome them. When panic attacks become a problem, it is usually in people with less self acceptance/ self like, they tend to dissapprove or dislike themselves. Maybe an underlying, limiting belief about self such as “I’m worthless” keeps them unconsciously wishing to punish themselves or self sabotage any attempts at changing it.
What are panic attacks?
They are not phobias, as phobias are a fear of something specific and identifiable outside of yourself, removal of which stops the symptoms of fear. But if you fear fainting in a public space or making a public spectacle of yourself in certain situations then your fear is a fear of panicking and is internally generated, caused by your own thoughts: “What if I faint? I’ll make such a fool of myself. What will others think of me?”
Panic attacks become inconsistent, their occurrence depending on a number of different circumstances, unpredictable and we don’t know why it happens or how you learned it. They always start with some event in childhood where we lost control of our bodies, usually due to illness, and fainted, were sick or had diarrhoea. This leaves us with a very negative emotional experience linked to a time and place. It is this memory of time and place linked with emotion, that becomes an unconscious pattern outside of our conscious control. And explains why they can be so scary.
What can be done?
Many people believe that, because they have had panic attacks for a while and have not been able to do anything about it, they are stuck with them and can’t change. But, whilst the change may not be immediate, and the person needs to put some effort in to change, panic attacks can be treated and life can return to normal. In Embodied Living therapy here are some of the processes that I look at to help people:
- education about the process of panic attacking
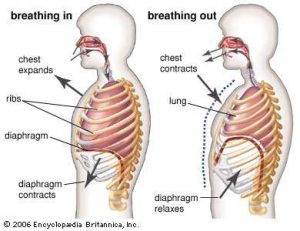
- assess hyperventilation/breathing and retrain breathing
- teach relaxation skills
- teach thinking skills and identify the trigger thought and learn to change/stop it
- identify the ‘dandelion root’ of limiting belief or event from early life and re-solution that
- develop witness mind to teach person to dissasociate and keep out of the panic
- install resources to help with managing emotional state and control the sympathetic nervous system: anchoring, resourceful self, cognitive distraction, SWISH, timeline intervention and memory resolution,
- tasking and practicing controlled exposure with resources
- building identity – ideal self – to build a more resourceful, resilient self this can have a huge impact on eradicating the panic attacks and helping people achieve their fully potential